Get Dexur’s Personalized Hospital Specific Presentation on Quality, Safety, Compliance & Education
Latest Dexur News
Dr.Alexander S. Mclawhorn is a top-ranked Physician with most experience for Hip & Knee Replacement in the United States according to Dexur’s analysis of Patient volumes. Research suggests that patient case volume and experience is positively correlated with better quality outcomes. Dexur is an approved purchaser of CMS claims data and the leading Quality Excellence platform for healthcare providers in the US. Dexur's data is trusted by healthcare leaders, media and top academic institutions such as Harvard.
Read moreDexur’s Free CMS Star Rating Measures, Time Periods, Time Lags and Methodology Poster
The Hospital CMS Star Ratings, designed to measure the quality of healthcare institutions, often presents hospitals with the challenging task of comprehending its intricate methodologies, encompassing performance periods, time lags, and specific weightages of different measures. Dexur, recognizing the complexity of these ratings, has identified that a significant portion of their interactions with hospitals revolves around elucidating these aspects. The need for clarity becomes particularly pronounced when considering that various teams within hospitals - from top-tier executives like the CEO, COO, CMO, CQO, and CNO to the Quality Departments - often have divergent understandings of how the Star Ratings function.
Read moreDexur’s 2024 CMS Star Rating Guidance in August 2023 is now available
Dexur’s 2024 Star Rating August 2023 Guidance is now available for hospitals and healthcare providers to review. Dexur has a 98% accuracy rate for its predictions in February. Our guidances, based on partial data, are less accurate but are still very useful to understand directionality, strengths, weaknesses and opportunities. Dexur customers may have a different guidance than what is shared below because they may have provided additional data to use in our guidance model.
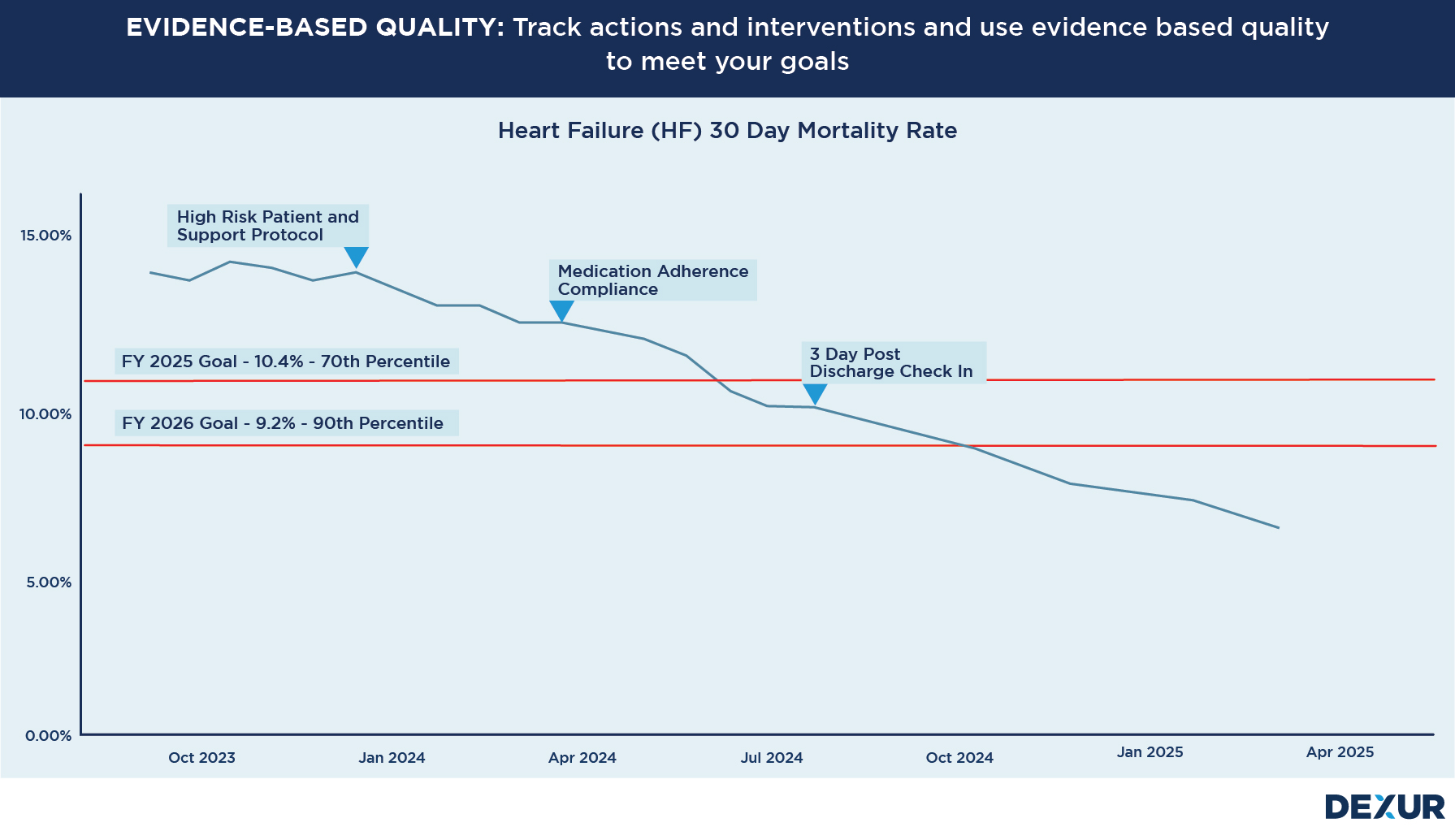
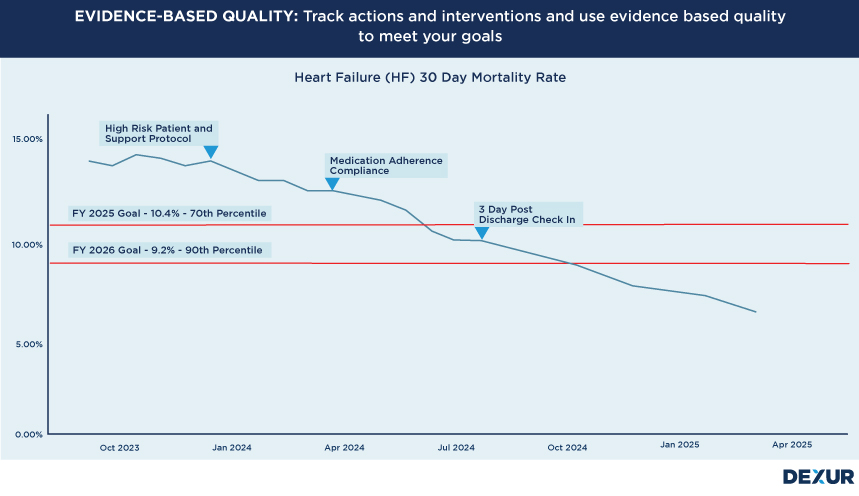
Read moreIn the vast expanse of the healthcare landscape, where patient care and hospital reputation are inextricably linked, hospitals frequently deploy a myriad of quality improvement initiatives, interventions, and actions. The goal is clear: to enhance the quality of care and ensure that patients receive the best possible treatment outcomes. However, there’s an underlining challenge that Chief Medical Officers (CMOs), Chief Nursing Officers (CNOs), and Quality Teams often grapple with — How do we know if these interventions are genuinely working?
Read moreNearly 30% of Readmissions are to a Different Hospital From the Index Stay
Hospitals face challenges in tracking CMS (Centers for Medicare & Medicaid Services) 30-Day readmissions due to the limitations of data. The 30-day Readmission measure is calculated based on the number of patients who are readmitted within 30 days of their initial hospital admission. However, hospitals lack access to comprehensive out-of-hospital information, making it difficult for them to track these measures accurately. Dexur is an approved purchaser of Medicare claims data and which allows it to evaluate patient outcomes, identify patterns and trends, and provide a more complete picture of healthcare utilization and performance. This data can be instrumental in identifying areas for improvement, developing strategies to reduce mortality and readmissions, optimizing resource allocation, and enhancing the overall quality of care.
Read moreDexur has a 98% predictive accuracy in 2023 CMS Star Ratings
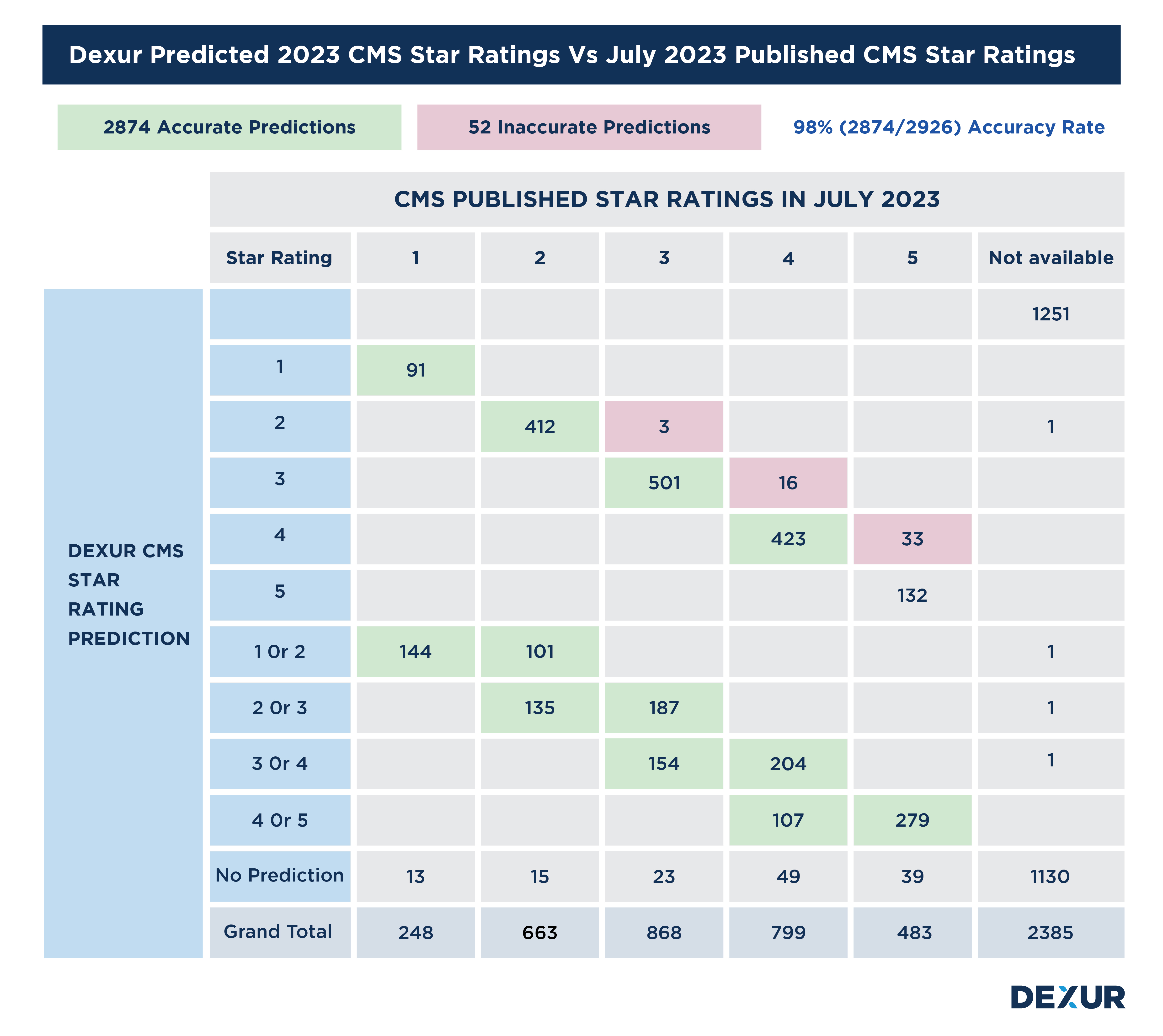
CMS just released its 2023 CMS Star Ratings on July 26, 2023. Based on the data files, released Dexur compared its CMS Star Rating predictions made in Jan / Feb 2023 to actual CMS published files and the details of comparison are shown below.
The key stats are given below:
-
Dexur made a prediction on 2926 Hospitals
-
Dexur correctly forecasted the CMS Star Rating in 2874 Hospitals (Green Highlighted in below table)
-
Therefore, Dexur has a 98% (2874/2926) predictive accuracy for 2023 CMS Star Ratings
-
52 Hospitals (Highlighted in pink in the below table) were incorrectly forecasted
Dexur's AI-Driven "Quality Advisor": Personalized Insights for Hospital Excellence
In the dynamic landscape of healthcare, where quality indicators like readmissions, mortality, CMS Star Rating, HRRP, and VBP determine both the quality of care and the financial health of institutions, having accurate, timely, and actionable insights can make a world of difference. This becomes even more crucial when hospitals aim to remain at the forefront of delivering superior patient care.
Read moreNearly 60% of Deaths for CMS Mortality Measures Happen Outside the Index Stay
Hospitals have a challenge in tracking CMS 30-Day Mortality measures because they try to monitor more real-time information using internal hospital data, which does not have out-of-hospital information used for 30-day mortality and readmission measures. However, Dexur is an approved purchaser of Medicare claims data and, therefore, can analyze the full patient journey that impacts measures such as 30-day mortality, 30-day readmissions, MSPB, and EDAC.
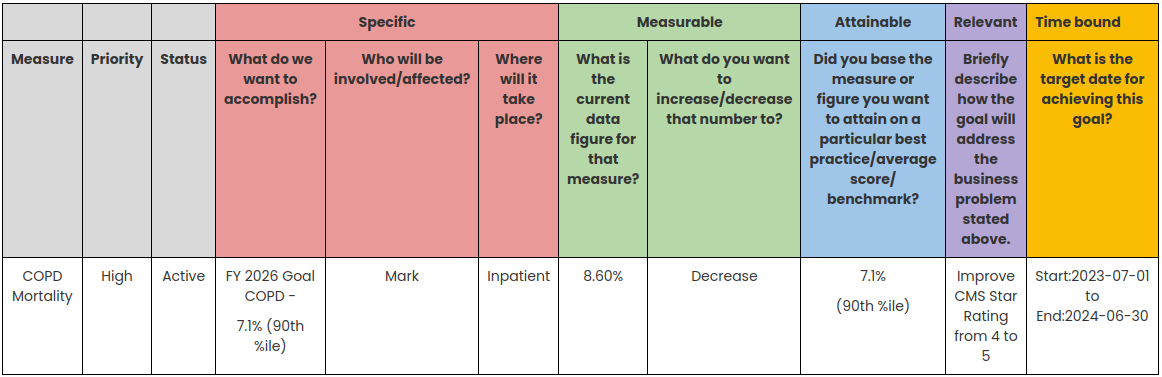
Read moreHow to Integrate CMS QAPI Goal Setting Frameworks for CMS Star Rating, VBP & HRRP
CMS QAPI (Centers for Medicare & Medicaid Services Quality Assurance and Performance Improvement) encourages healthcare organizations to establish and monitor quality improvement goals. These goals can align with the metrics and measures used in CMS quality programs, including Star Ratings, VBP and HRRP. By setting specific goals to improve performance on quality measures that impact Star Ratings VBP and HRRP, healthcare organizations can directly link their compliance efforts to the desired outcomes in CMS quality programs.
Read moreHow Dexur Helps Hospitals Achieve Quality Excellence
Hospitals are often surprised by the outcomes of CMS Programs and struggle to improve CMS Star Ratings and Payouts and reduce Penalties. This is because of four reasons:
- Lack of out-of-hospital data (e.g., for 30-day readmissions and mortality)
- Lack of expert resources to update changing quality measure algorithms
- Little room for error in final measure scores
- Lack of scale and budget to invest in modern software.
In the pursuit of improving healthcare quality and patient outcomes, the Centers for Medicare & Medicaid Services (CMS) rely on various measures to evaluate the performance of hospitals and healthcare providers. Two crucial indicators that have garnered significant attention to assess hospital performance are readmission and mortality rates. These measures are crucial in measuring Hospitals’ performance in various CMS quality programs. For instance, readmissions and mortality measures constitute 44% weightage in the calculation of CMS Star Ratings, and readmissions are the sole driver of the Hospital Readmissions Reduction Program (HRRP).
Read moreNavigating the complexity of CMS programs - CMS Star Ratings, Hospital Readmission Reduction Program (HRRP), Value-Based Purchasing (VBP), and Medicare Spending per Beneficiary (MSPB) - often brings unforeseen challenges for healthcare providers. Unpredictability in CMS Star Ratings, HRRP penalties, and VBP payouts can create disruption and uncertainty.
Read moreDexur’s Best Practices Research to Drive Quality
Dexur’s cutting-edge data, research, analytics, and software capabilities serve as the foundation for effective quality improvement strategies. An integral part of our offerings is our dedicated research team, which continuously investigates best practices to enhance quality outcomes that feed into significant programs like CMS Star Rating, CMS Hospital Readmission Reduction Program (HRRP), and CMS Value-Based Purchasing (VBP).
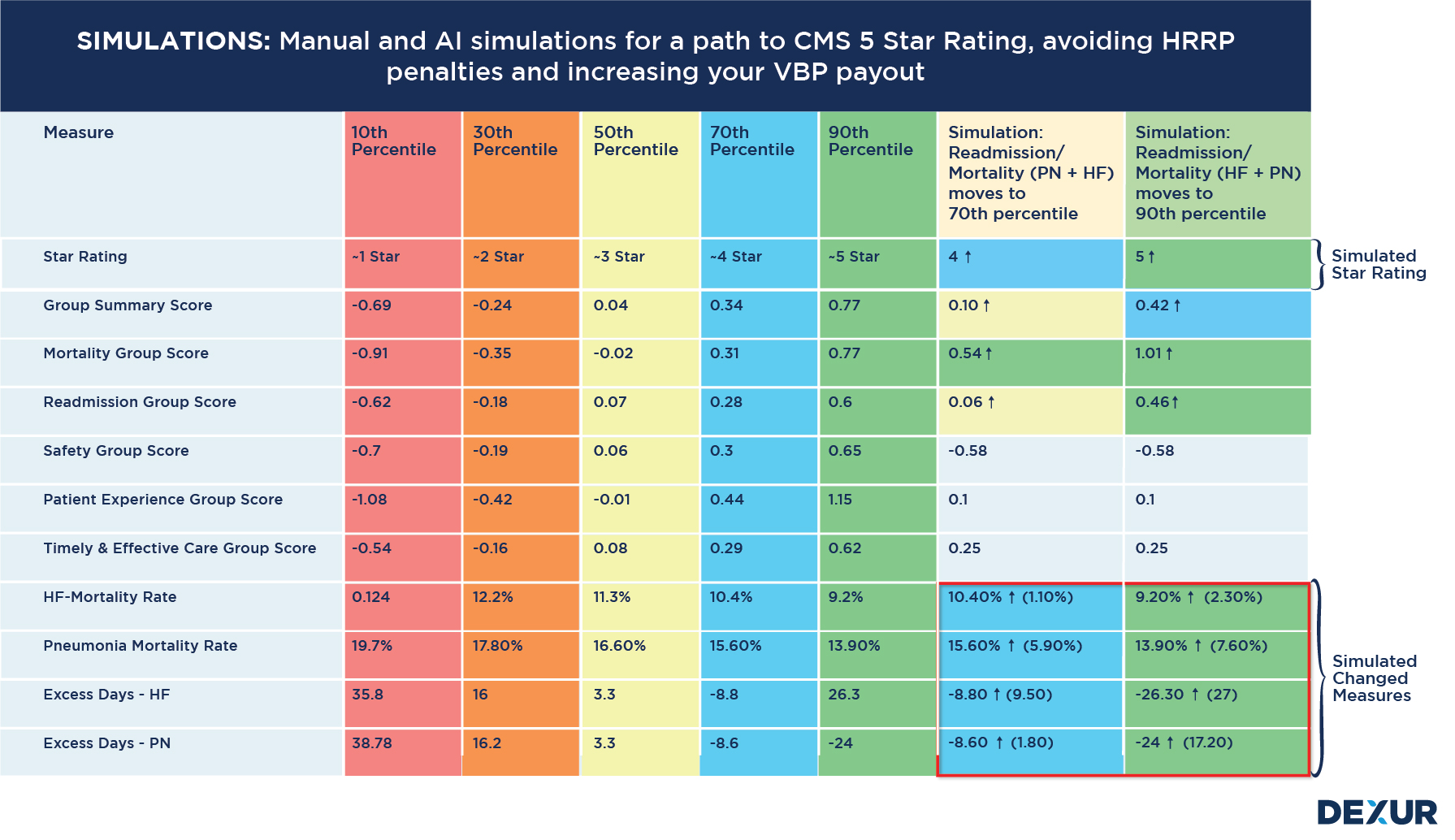
Read moreDexur Simulations: Your Predictive Path to Quality Excellence
Welcome to Dexur, your guide to mastering complex Healthcare quality and CMS programs and metrics. At Dexur, we understand the importance of foresight in a rapidly evolving healthcare landscape. That's why we offer not just predictive analytics, but powerful simulation capabilities that help you visualize your path to CMS program excellence.
Read moreDexur Evidence Based Quality Management
At Dexur, We don't just provide insights; we offer a holistic solution that helps you implement, track, and understand the impact of various interventions, protocols, actions, and best practices to exceed your quality goals.
Read moreDexur Goal Setting and Tracking: Streamlining Healthcare Quality Improvement
Welcome to Dexur, your ally in unlocking the power of healthcare data and predictive analytics. Our sophisticated platform doesn't stop at providing insights and simulations. Dexur also empowers healthcare organizations to set, track, and achieve their goals for improving quality outcomes.
Read moreDexur believes that efficient data management is key to making informed decisions, and that's why we offer a comprehensive Measures & Data feature. This innovative solution allows you to consolidate all key measures impacting your quality, safety, and compliance programs in one place, integrated seamlessly with both internal and external data sources.
Read moreThe healthcare sector is rapidly advancing, yet many hospitals are still relying on outdated incident management software that lacks modern technological capabilities, integration with quality management, and cost-effectiveness. Dexur’s Unified Quality and Incident Management Platform emerges as a modern, integrated, and cost-efficient solution for healthcare organizations.
Read moreDexur’s Provider Quality Analytics Solutions for Life Sciences Organizations
Dexur's anonymized claims database forms the bedrock of our disease burden data and dashboards. Our data collection and analysis processes are rigorous, ensuring we offer valuable insights into specific diseases, like Diabetes or Chronic Kidney Disease. This information includes vital metrics such as total cost of care, readmission rates, mortality, nursing home costs, and length of stay, among others.
Read moreDexur Quality Outcomes Predictions: Your Future in Healthcare, Predicted Today
At Dexur, we turn complex healthcare data into comprehensible insights that you can leverage to improve patient outcomes, optimize hospital performance, and anticipate future challenges. Our unique blend of sophisticated data science and deep understanding of healthcare systems gives you the edge in an increasingly data-driven world.
Read more