Dexur Hospital & Provider Quality Data Suite & Services
Readmissions & CMS HRRP Forecasts, Predictions & Analytics
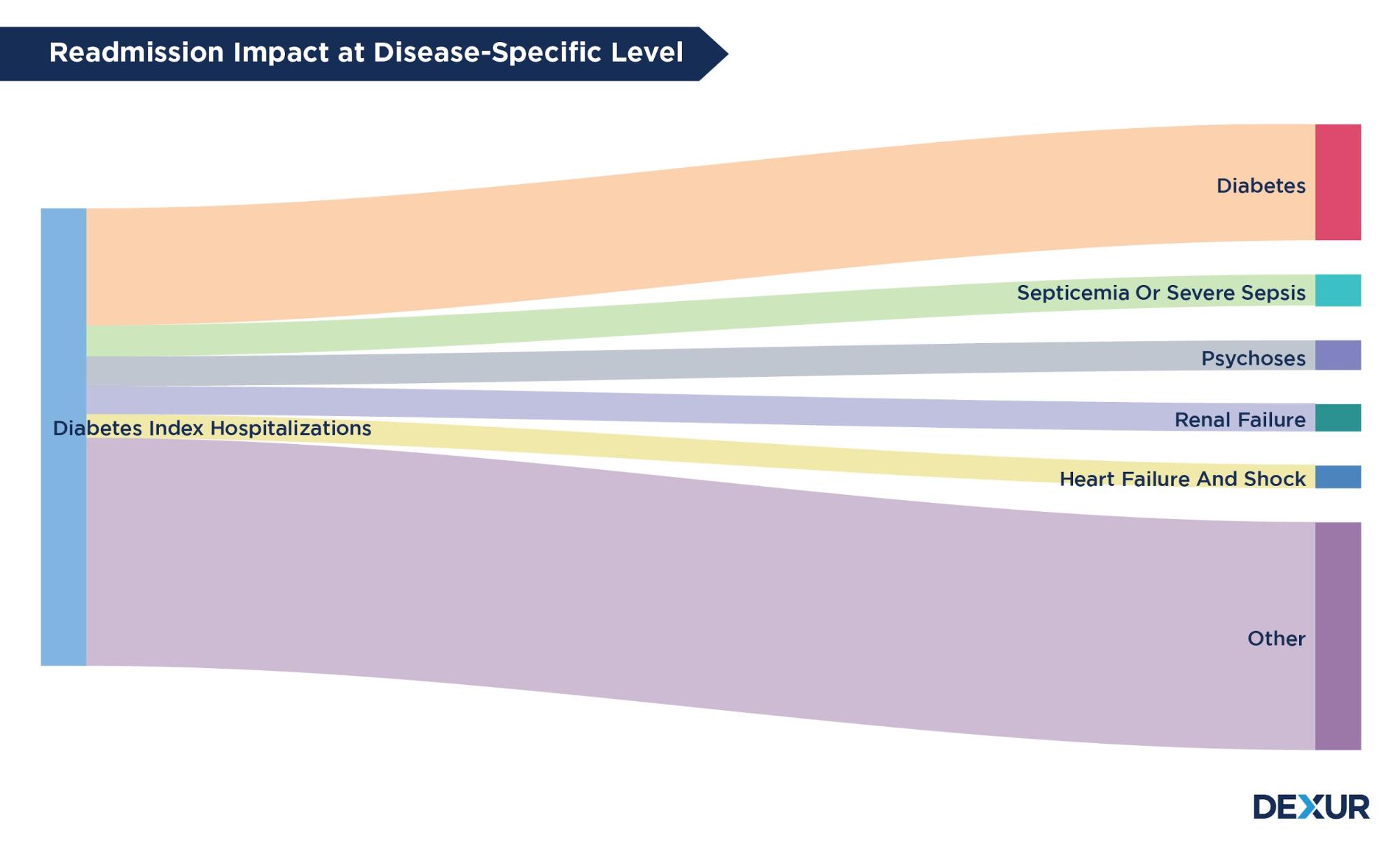
Dexur predicts CMS HRRP penalties 1 to 3 years in advance of CMS Published data using Medicare claims data, replication of the HRRP methodology and Dexur’s forecasting methods. Further, Dexur also boils the ocean to identify all Real World Evidence (RWE) Risk factors that drive higher readmissions and penalties for each measure (E.g. COPD, Heart Failure…). Dexur’s HRRP and RWE Risk factor analysis helps hospital proactively predict and improve readmissions to drive quality and value outcomes.
CMS Star Rating Forecasts, Predictions & Analytics
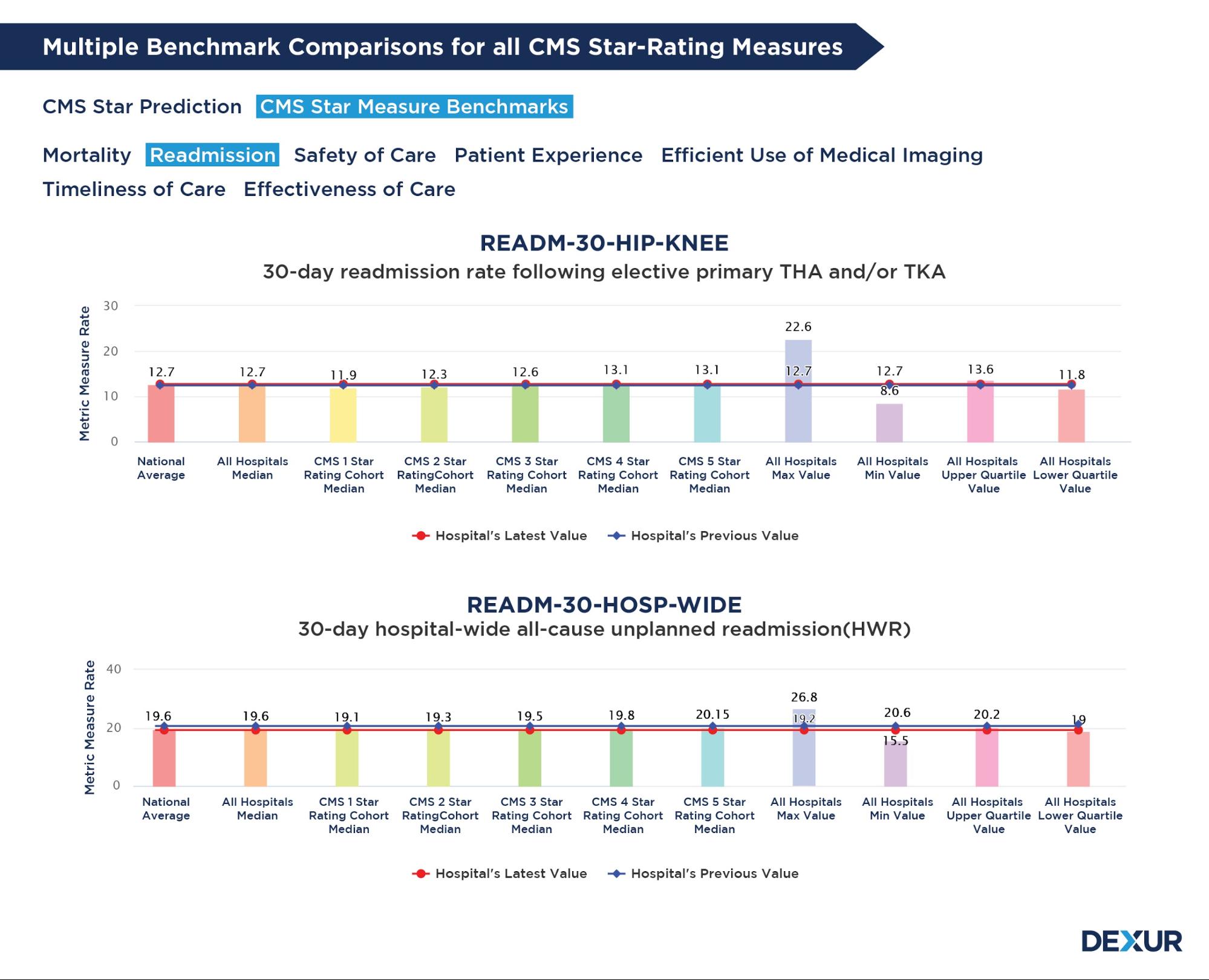
Check your CMS Star Rating Prediction for the upcoming year. Assess each measure incorporated to carry out the rating calculations and improve performance in heavily weighted categories. Dexur calculates trends for each of the measure groups:
- Mortality
- Safety of Care
- Readmission
- Patient Experience
- Effectiveness of Care
- Timeliness of Care
- Efficient Use of Medical Imaging
CMS Value Based Purchasing (VBP) Forecasts, Predictions & Analytics
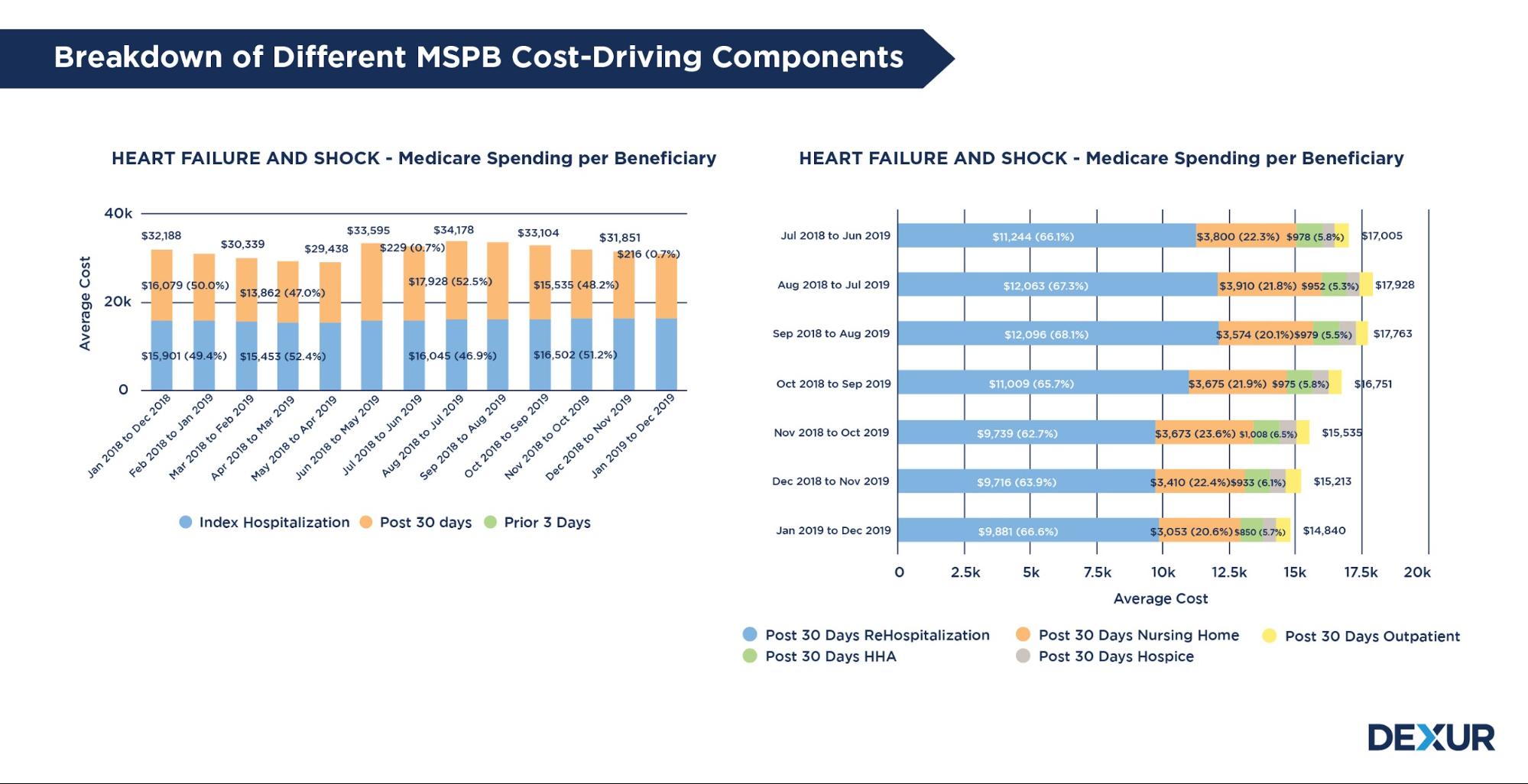
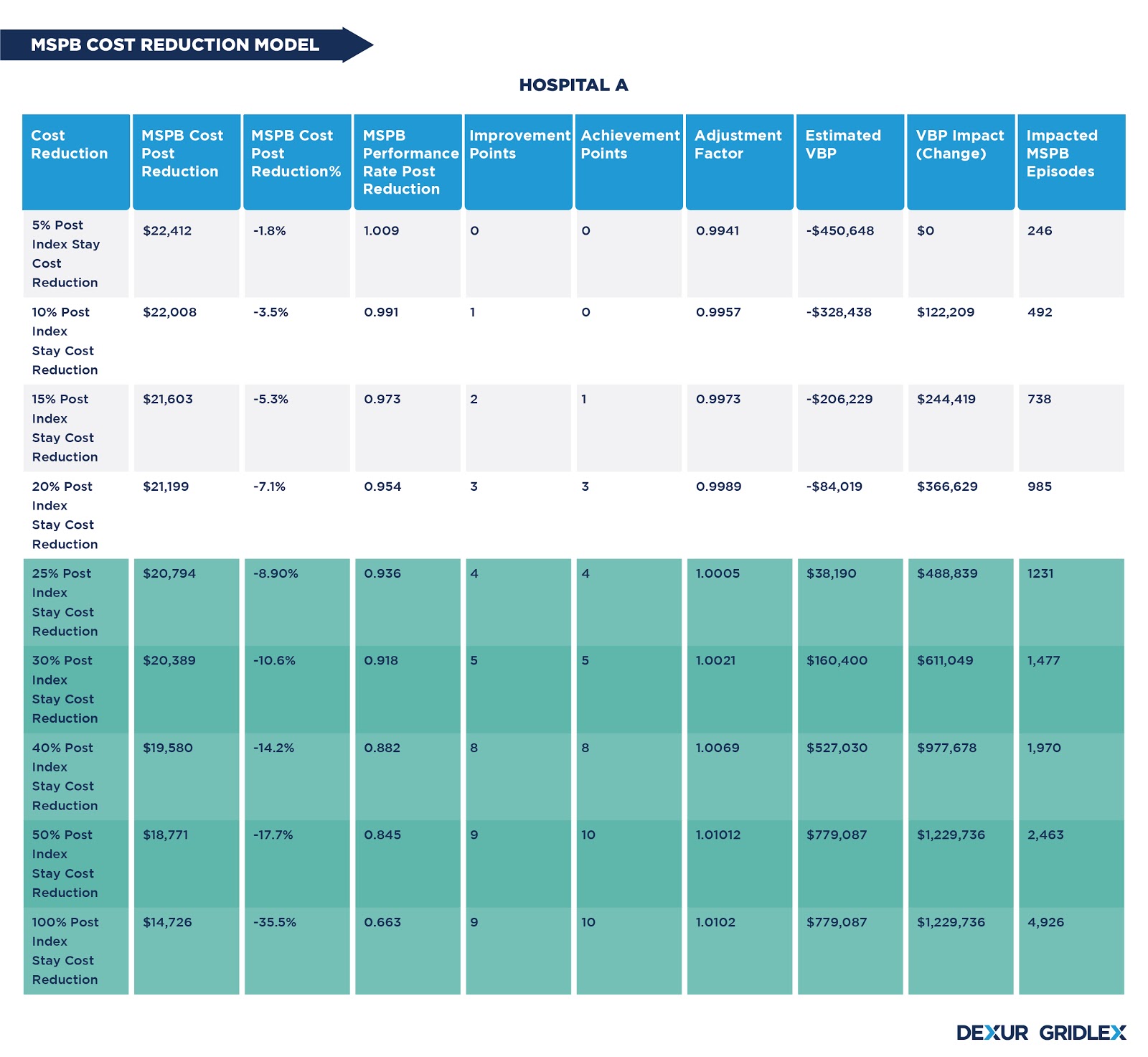
Track and evaluate Value-Based Purchasing domain measures ahead of performance period evaluation for the latest Fiscal Year. Dexur assembles VBP measure scores for all the domains; Clinical Care, Efficiency and Cost Reduction, Safety and Person and Community Engagement. Medicare Spending per Beneficiary cost per episode is broken down to identify cost-driving components like post-acute care costs..
Hospital Acquired Conditions Forecasts, Predictions & Analytics
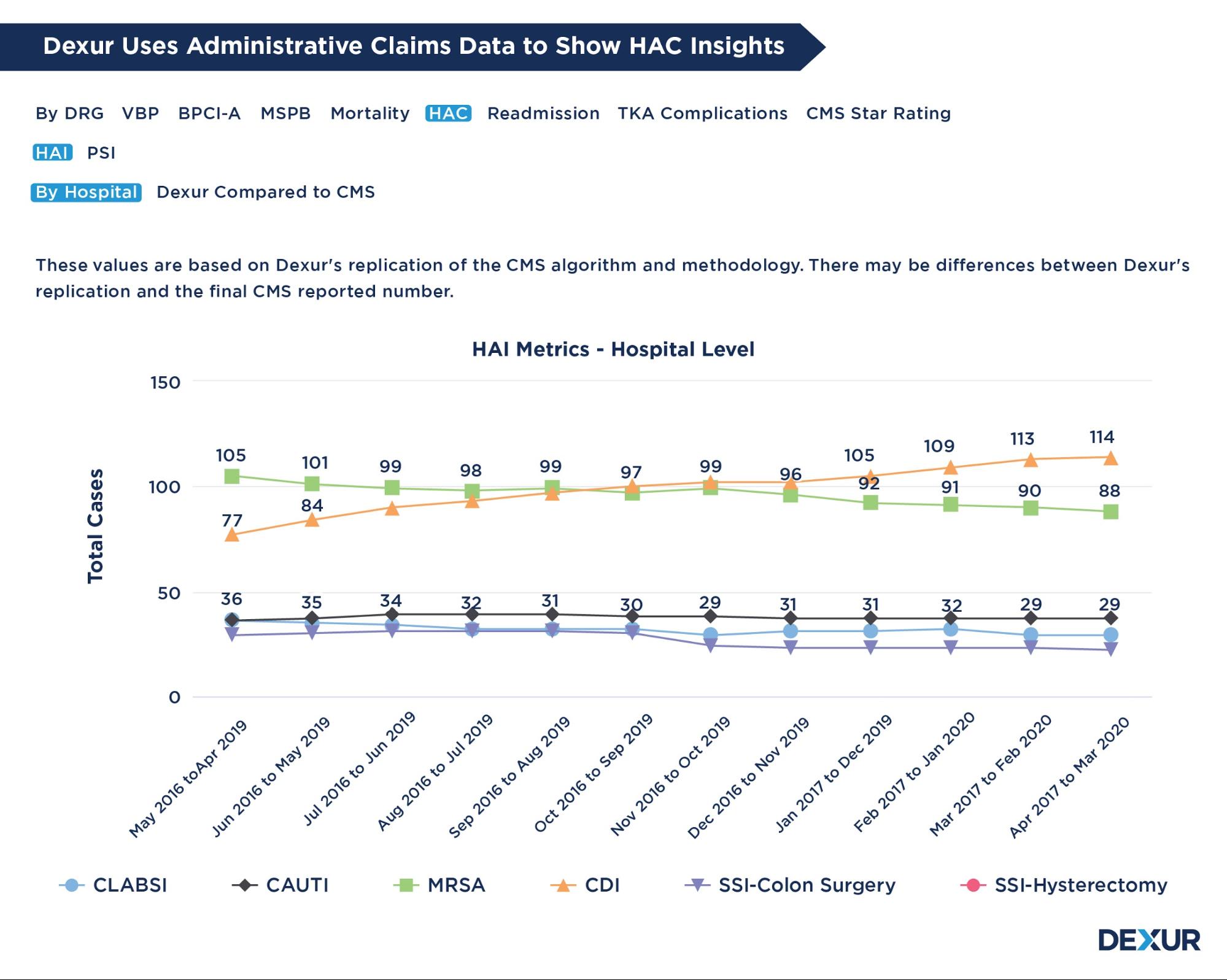
Gauge all set of measures under the Hospital-Acquired Condition Reduction Program (HACRP), each of the Hospital Associated-Infections (HAI) and a composite PSI-90 (Patient Safety Indicator) evaluation. The HAI measures included are:
- Central Line-associated Bloodstream Infections (CLABSI)
- Catheter-Associated Urinary Tract Infection (CAUTI)
- Methicillin-resistant Staphylococcus aureus (MRSA)
- Surgical Site Infection (SSI)
- Clostridium difficile Infection (C. Diff)
CMS BPCI Conditions Forecasts, Predictions & Analytics
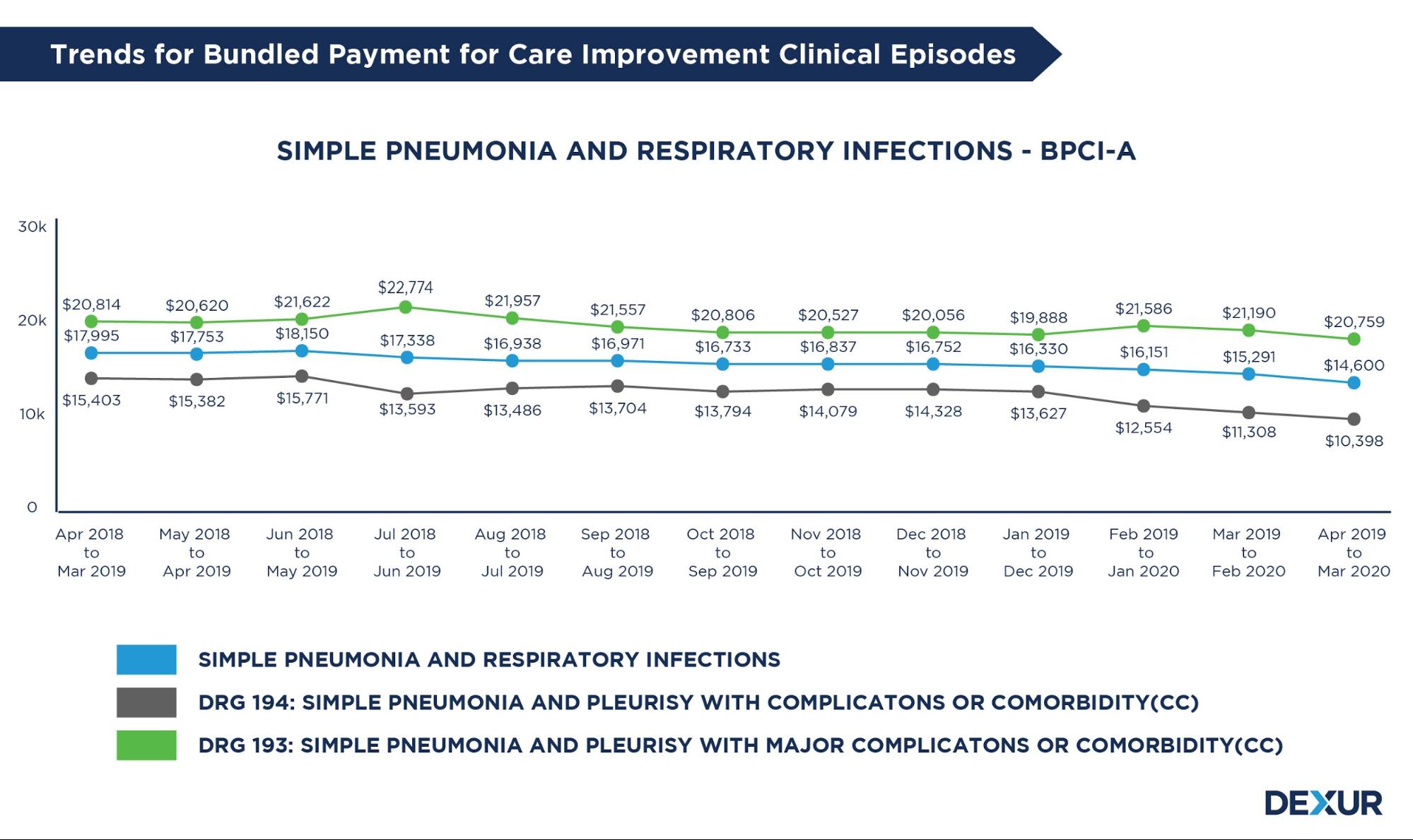
Evaluate trends for each clinical episode your hospital has enrolled for, along with projected estimates for prospective episodes. The Bundled Payments for Care Improvement Advanced (BPCI Advanced) Model is a new iteration of the Centers for Medicare & Medicaid Services CMS and the Center for Medicare and Medicaid Innovation continuing efforts in implementing voluntary episode payment models.Dexur calculates bundled payment for all 31 inpatient clinical episodes covered under BPCI-A
Readmission and Mortality rates are hospital quality measures that reflect dimensions of quality in patient care. Dexur calculates Readmission and Mortality rates for all CMS measures and helps Hospitals improve their outcomes for various cost and quality programs.
Dexur Simulators and Calculators to manage CMS Quality programs
To help healthcare providers in managing costs and monitoring CMS quality programs, Dexur has developed several simulators and calculators that provide insights and suggest useful scenarios to administer costs and quality outcomes. Dexur provides Simulators for the following quality programs:
- Value Based Purchasing (VBP)
- Medicare Spending Per Beneficiary (MSPB)
- Hospital Readmissions Reduction Programme (HRRP)
- Hospital Acquired Conditions (HAC)
- CMS Star Rating
Dexur Hospital Quality Benchmarks
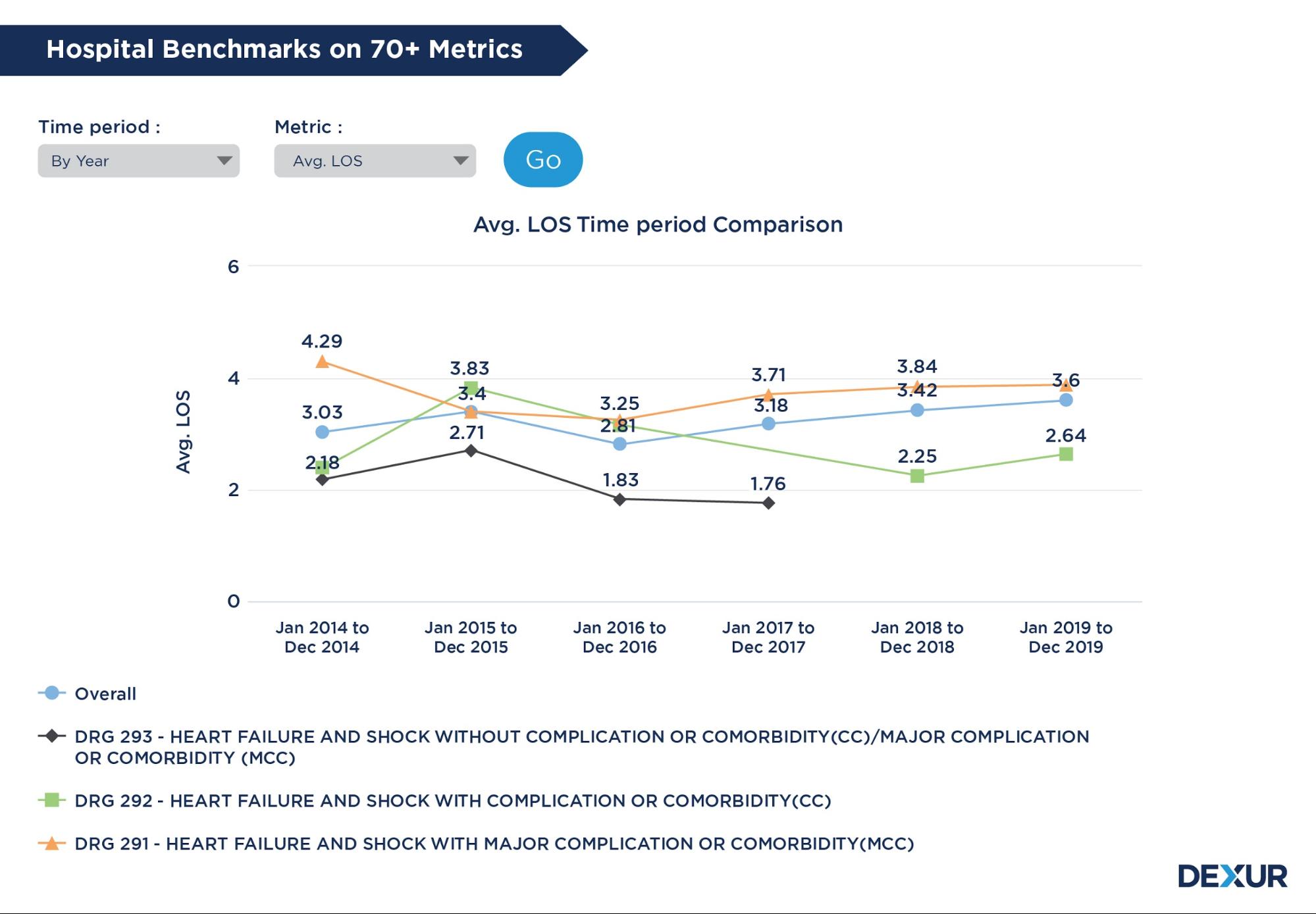
Leverage data analytics on 70+ metrics like readmissions, mortality, length of stay, volume, cost of care, and more. Dexur distributes data into quarterly, yearly, and rolling three year time periods to chart a clearer overview of trends. The data is risk-adjusted at a DRG level and for performance-driven metrics. Cost of Care data for each metric is taken over 30, 60, 90 days and 1 year period to show trends in post-acute expenditure and discharge rates.
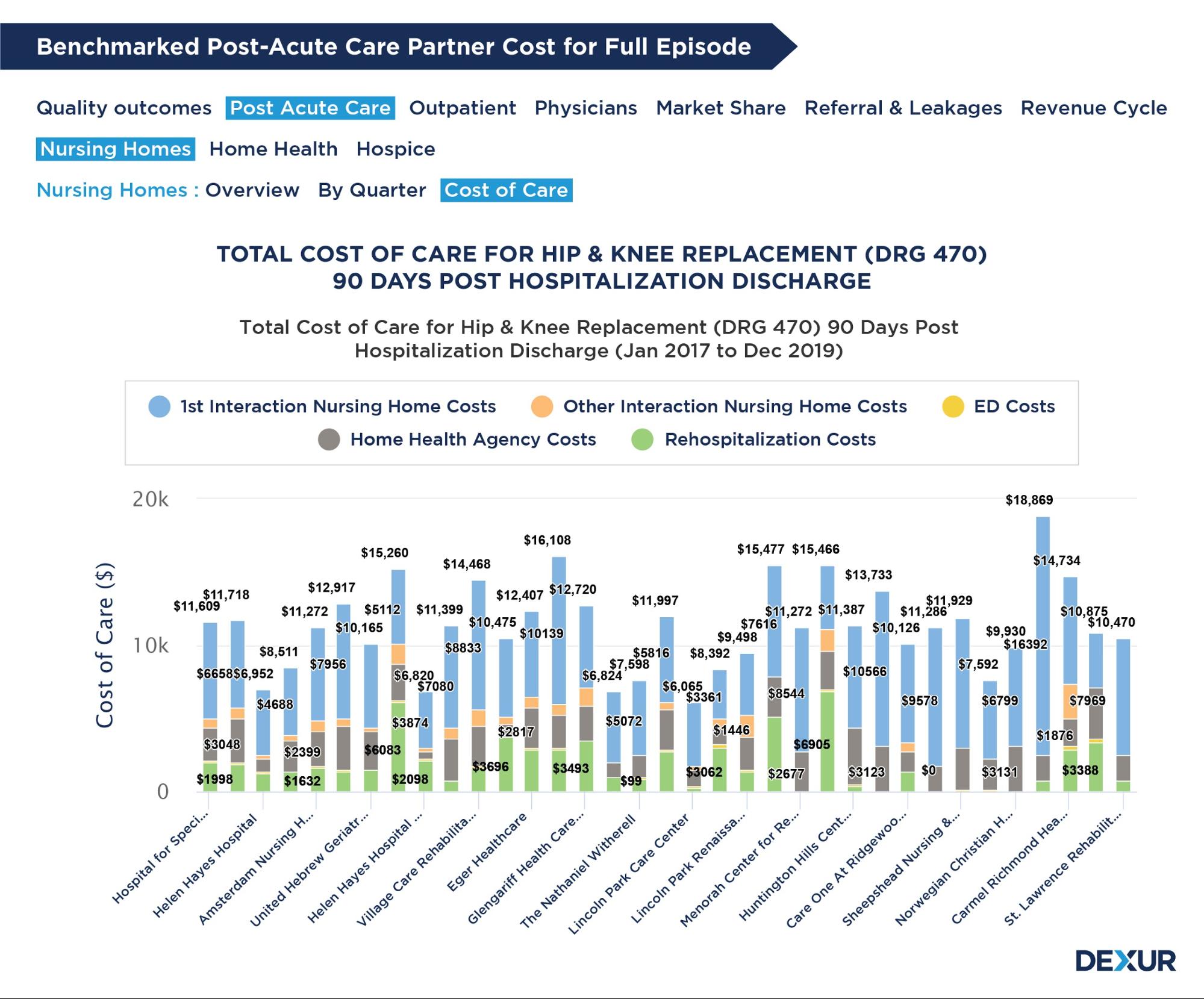
Dexur's Post Acute Care Analytics and Insights
Track patients’ journey before admission & post-discharge by analyzing SNF, HHA & Hospice referrals, cost of care & readmissions, in conjunction with outpatient claims and payments. Dexur calculates SNF discharge rates for the Medicare Spending Per Beneficiary (MSPB). Post-acute care costs significantly impact a facility’s / physician’s MSPB average; a lower post acute-care facility Discharge Rate will help reduce MSPB average and thereby optimize the incentives.