In Most Louisiana Hospitals, Post-Surgical ABSSSI-Related 30-Day Readmission Rates Exceed National Average
In Acute Bacterial Skin and Skin Structure Infections (ABSSSI)
Get Dexur’s Personalized Hospital Specific Presentation on Quality, Safety, Compliance & Education
By: James Pitt May. 04, 2018
A Dexur analysis examined 30-day readmission rates among Medicare inpatients discharged after surgery in Louisiana and found that most Louisiana hospitals had ABSSI-related 30-day readmission rates higher than the national average. The analysis was limited to hospitals with over 1,000 CMS inpatient discharges per year.
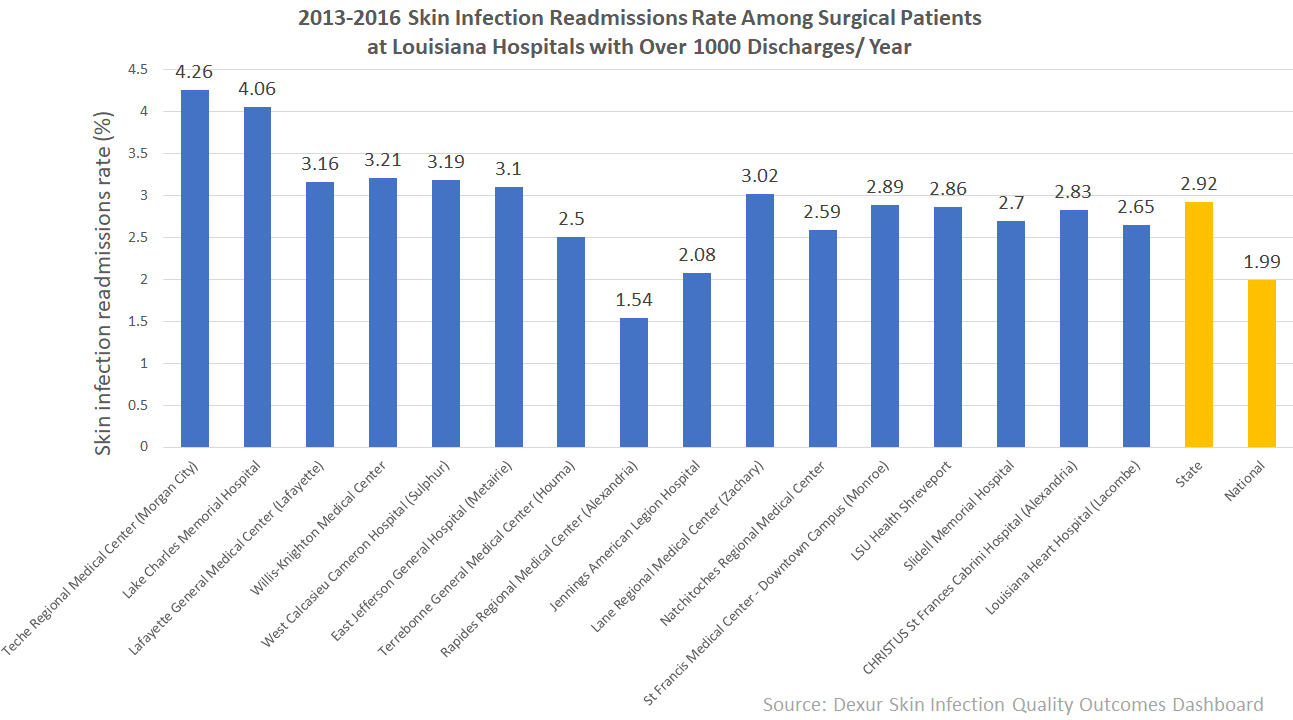
Large hospitals with lower 30-day readmission rates than the statewide average included Rapides Regional Medical Center (Alexandria), Terrebonne General Medical Center (Houma), Jennings American Legion Medical Center, Natchitoches Regional Medical Center, St. Francis Medical Center's downtown campus (Monroe), LSU Health Shreveport, Slidell Memorial Hospital, CHRISTUS St. Francis Cabrini Hospital (Alexandria), and Louisiana Heart Hospital (Lacombe), which closed in February 2017.
Skin infections are a particular challenge in Louisiana. Warm and humid regions are associated with skin infections. A particular serious category of skin infection is ABSSSI, acute bacterial skin and skin structure infection. A variety of infections can cause this condition. Most notorious is methicillin-resistant staphylococcus aureus (MRSA).
Louisiana's 30-day skin infection readmission rate for surgical patients is 2.92%, much higher than the US average 1.99%. Fortunately, according to the CDC, “Although MRSA is still a major patient threat... MRSA infections in healthcare settings are declining. Invasive MRSA infections that began in hospitals declined 54% between 2005 and 2011, with 30,800 fewer severe MRSA infections.”
Another well-known cause of complicated skin infections in Louisiana is Vibrio vulnificus. This rare but dramatic bacterium receives extensive press coverage for its rapid onset and high mortality. According to the Baton Rouge Advocate, there are 10 to 15 cases of Vibro vulnificus in Louisiana per year. V. vulnificus is thought to be growing more common, and had a 17% mortality rate in Louisiana between 1988 and 2013. Worldwide, Huang et. al 2016 estimated V. vulnificus's 5-year mortality rate is as high as 37%. Unlike MRSA, this infection is rarely associated with nosocomial infections of surgical wounds.
ABOUT THE AUTHOR
