Septic Shock Involved in Nearly Half of Charlotte, NC In-Hospital Deaths in DRG 871 Patients
In Sepsis
Get Dexur’s Personalized Hospital Specific Presentation on Quality, Safety, Compliance & Education
By: James Pitt Aug. 02, 2018
Sepsis is a condition in which an infection triggers a bodywide response. Diagnostic criteria include elevated body temperature, heart rate, and respiratory rate, according to the Mayo Clinic. Terminology around sepsis can be blurry, and has shifted over time. The latest edition of the Merck Manual defines septic shock as sepsis that causes dangerously low blood pressure.
To study the impact of septic shock on overall sepsis mortality, Dexur analysts examined data from five hospitals in Charlotte, South Carolina. The most common sepsis diagnosis in Medicare-eligible inpatients is DRG 871, septic shock with major complications or comorbidities but with less than 96 hours of mechanical ventilation.
In Charlotte, septic shock accounted for nearly half of in-hospital deaths in patients classed under DRG 871. At Carolinas Medical Center's main Charlotte location, 19% of DRG 871 patients died in-hospital. Only 10% of DRG 871 patients without septic shock died in-hospital.
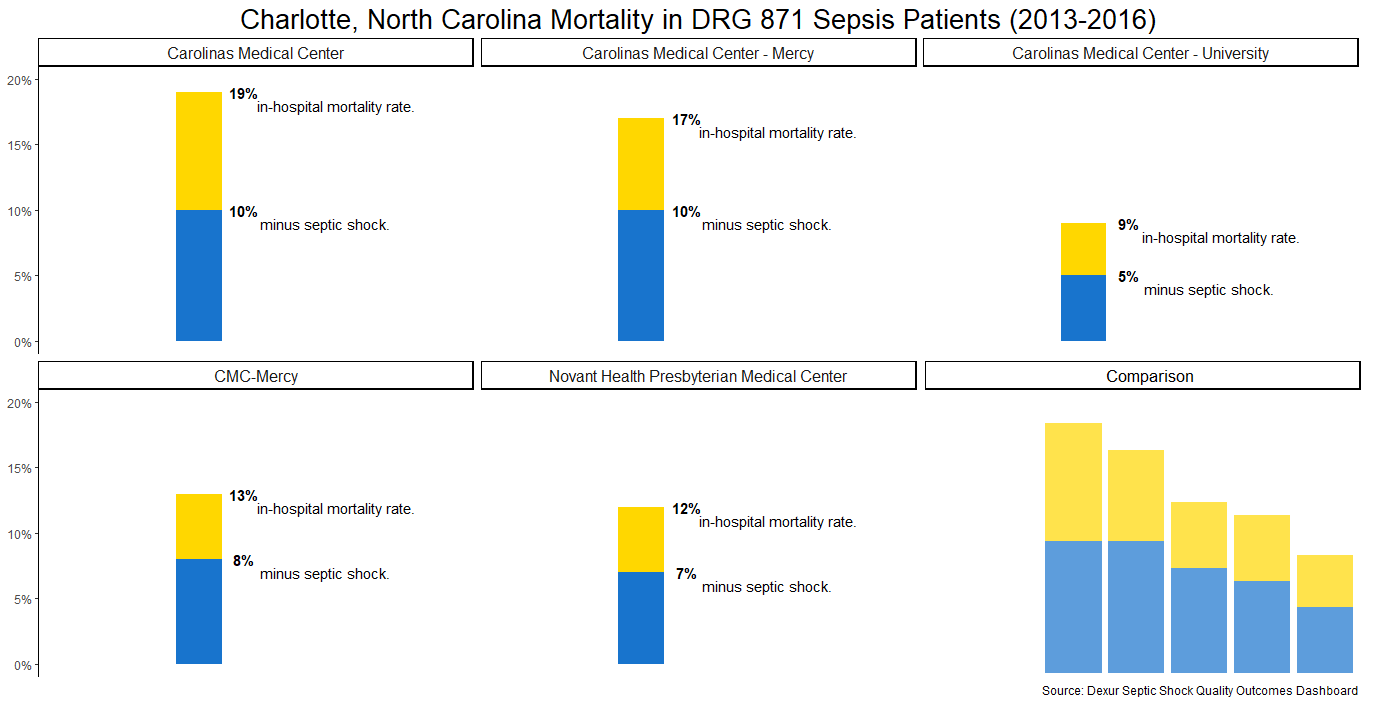
The smallest gap was at CMC-Mercy (2001 Vail Ave), not to be confused with the Carolinas Medical Center - Mercy listed above, which is located at 10628 Park Road and has since been renamed Carolinas HealthCare System Pineville). At CMC-Mercy, the overall mortality rate in DRG 871 sepsis patients was 13%. In DRG 871 patients without septic shock, the mortality rate fell to 8%.
Like hypovolemic shock, septic shock involves an initial drop in blood pressure. For this reason, the Surviving Sepsis bundle (recommended by CMS) involves fluid resuscitation. However, too much fluid increases subsequent mortality. Dexur has reported extensively on fluid imbalance in sepsis.
DEXUR PRO MEMBERS GET ACCESS TO:
- Total DRG Discharges
- Total Septic Shock Discharges at DRG
- % of Septic Shock Discharges at DRG
- Mortality Rates at DRG
- Mortality Rates without Septic Shock at DRG
- Mortality Rates with Septic Shock at DRG
- Difference in Mortality Rates with & without Septic Shock
- State Difference in Mortality Rates with & without Septic Shock
- National Difference in Mortality Rates with & without Septic Shock
For DRG 870 and DRG 871, at the following hospitals:
- CMC Mercy (Charlotte, North Carolina)
- Carolinas Medical Center Mercy (former, now Carolinas Healthcare Pineville) (Charlotte, North Carolina)
- Carolinas Medical Center (Charlotte, North Carolina)
- Carolinas Medical Center - University (Charlotte, North Carolina)
- Novant Health - Presbyterian (Charlotte, North Carolina)
ABOUT THE AUTHOR
